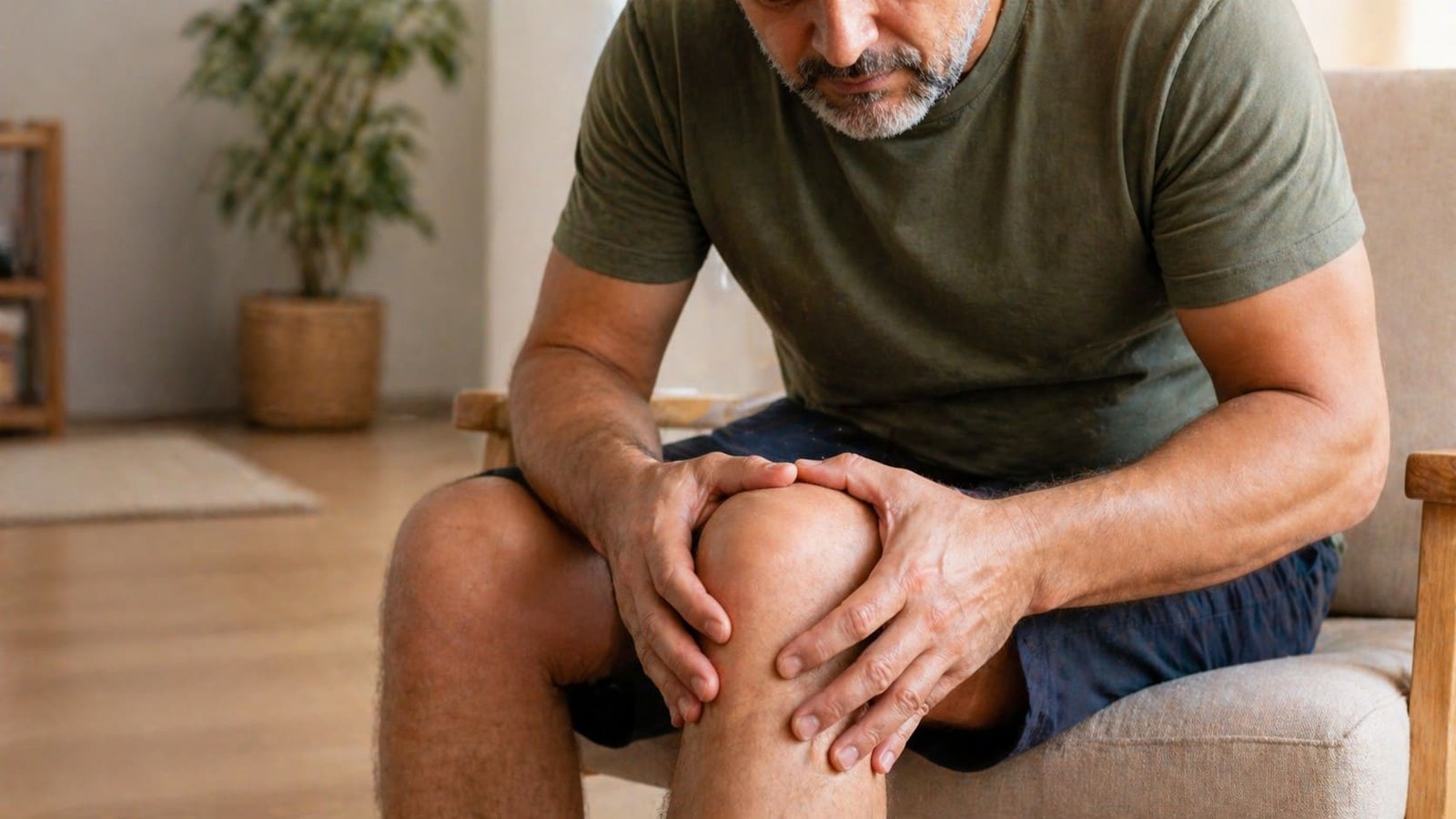
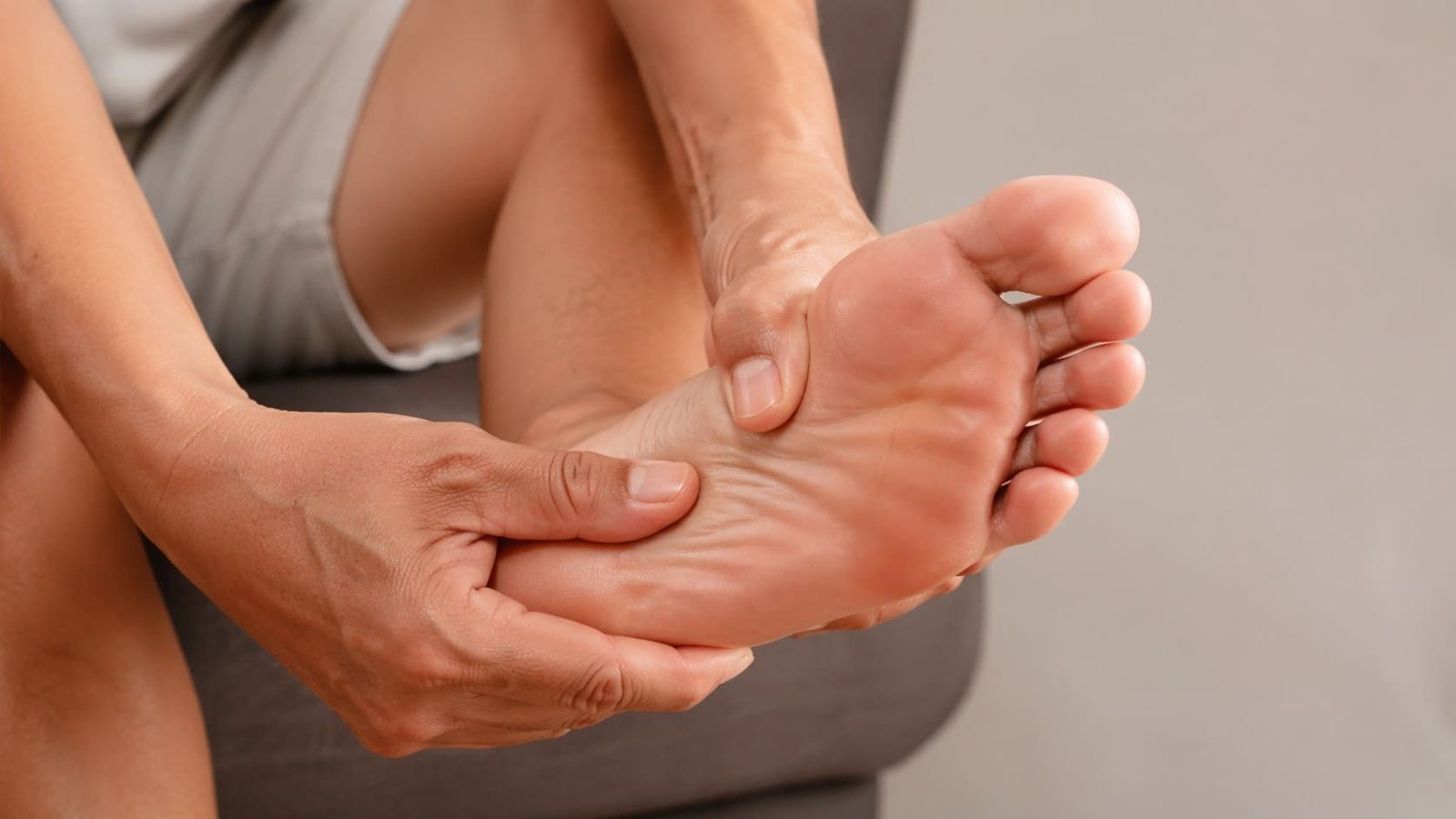
Morning stiffness, reduced range of motion, and joint discomfort that wasn't there a few years ago are your body's early warnings — here's what they mean and what to do.
Joints are one of those parts of the body that most people don't think about until they start causing problems. And by the time joint pain is significant enough to demand attention, the underlying damage — cartilage thinning, synovial fluid depletion, chronic inflammation — has typically been accumulating for months or years. The early warning signs are real, measurable, and often dismissed as normal aging long before they become genuinely limiting.
Osteoarthritis — the most common form of joint disease — affects over 32 million Americans and is the leading cause of disability in adults. It develops through a gradual process of cartilage breakdown that begins years before pain becomes constant. The earlier that process is recognized and addressed, the more options are available and the more progress can be slowed.
This article covers the most common signs that your joints are under strain, explains the biology behind each one, and outlines what natural support strategies are most relevant at different stages of joint health decline.
How Healthy Joints Work — and What Changes With Age
A healthy joint consists of several structures working together: cartilage (the smooth, shock-absorbing tissue covering the ends of bones), synovial fluid (the viscous lubricant that fills the joint space), the synovial membrane (which produces synovial fluid), ligaments (connective tissue holding bones together), and surrounding muscles and tendons that support and move the joint.
In a healthy joint, cartilage allows bone surfaces to glide smoothly against each other with minimal friction. Synovial fluid — rich in hyaluronic acid — maintains the lubrication that enables this gliding and delivers nutrients to cartilage, which has no direct blood supply of its own.
With age, activity-related wear, injury history, excess body weight, and inflammatory dietary patterns, this system degrades in predictable ways. Cartilage thins and becomes less resilient. Synovial fluid loses its viscosity and hyaluronic acid concentration. The inflammatory environment within the joint increases. Bone begins to remodel in response to altered load distribution. Each of these changes produces recognizable symptoms — and each has a window during which appropriate support can make a meaningful difference.
10 Signs Your Joints Need Support
1. Morning Stiffness Lasting More Than 15 Minutes
Some degree of morning stiffness is normal — joints that have been still overnight need a few minutes to warm up and redistribute synovial fluid. What's worth paying attention to is stiffness that persists beyond 15 minutes after getting up. This duration suggests that synovial fluid quality or quantity has declined enough that lubrication is inadequate at rest, requiring extended movement before the joint functions normally. In osteoarthritis, morning stiffness is typically brief (under 30 minutes) and improves with gentle activity — distinguishing it from the prolonged morning stiffness of inflammatory arthritis like rheumatoid arthritis, which often lasts an hour or more.
2. Joint Pain That Worsens With Activity
Pain that increases with use — walking up stairs, gripping objects, bending down — and improves with rest is one of the most characteristic patterns of mechanical joint wear. It reflects thinning cartilage that provides less cushioning under load, and increased bone-on-bone contact during weight-bearing movement. This is distinct from inflammatory joint pain, which often improves with movement and worsens with prolonged rest. Activity-worsening pain that develops gradually over months is a reliable early indicator of cartilage changes worth addressing proactively.
3. Clicking, Popping, or Grinding Sensations
Occasional joint clicking from gas bubbles in synovial fluid is normal and harmless. What's more significant is a consistent grinding or crunching sensation — called crepitus — particularly when it is associated with discomfort. Crepitus occurs when cartilage surfaces are no longer smooth enough to glide silently against each other during movement. Research has found that crepitus in the knee, particularly when combined with pain, is a clinically useful early indicator of cartilage degradation. Consistent crepitus without pain is worth monitoring; crepitus with pain warrants proactive joint health attention.
4. Reduced Range of Motion
Difficulty fully straightening or bending a joint — reaching the full range of motion that was previously effortless — reflects either structural changes in the joint (cartilage loss changing joint geometry, bone spurs forming at joint margins) or protective muscle guarding around a painful joint. Both represent meaningful changes from baseline function. Many people adapt to reduced range of motion so gradually that they don't notice it until comparison with their younger selves reveals how much mobility has declined. Regular yoga, stretching, or functional movement assessments are practical ways to monitor range of motion over time.
5. Joint Swelling After Activity
Swelling around a joint following physical activity — the knee that puffs up after a long walk, the knuckles that feel thicker after repetitive hand use — reflects inflammatory fluid accumulating in response to mechanical stress on a compromised joint. The synovial membrane produces excess fluid in response to cartilage breakdown products and inflammatory signals, causing the characteristic puffy appearance and sensation. Occasional post-activity swelling in a joint with known wear is expected; progressive worsening swelling after less and less activity is a signal that the inflammatory burden within the joint is increasing.
6. Warmth or Tenderness Around a Joint
Warmth and tenderness to touch around a joint reflect active local inflammation. In osteoarthritis, this typically occurs during flare periods — often triggered by overuse, weather changes, or dietary inflammation. Persistent warmth and tenderness that doesn't resolve with rest may indicate a more active inflammatory process worth investigating medically. The inflammation itself, when chronic, accelerates cartilage degradation — creating a self-reinforcing cycle where joint damage drives inflammation, which drives further damage.
7. Pain That Affects Sleep Quality
Joint pain that wakes you at night, or that makes finding a comfortable sleeping position difficult, represents a meaningful escalation from daytime-only discomfort. Nighttime joint pain is more commonly associated with inflammatory joint conditions, though osteoarthritis patients frequently report disrupted sleep from joint discomfort — particularly hip and knee pain that is exacerbated by certain sleeping positions. Sleep disruption from joint pain creates a secondary cycle: poor sleep increases systemic inflammation, which worsens joint pain, which disrupts sleep further.
8. Weakness in the Muscles Around the Joint
Joint pain causes reflexive inhibition of the muscles surrounding the affected joint — the body's protective mechanism to reduce load on a painful structure. Over time, this protective inhibition leads to measurable muscle weakness and atrophy around the joint. Quadriceps weakness relative to the hamstrings, for example, is both a consequence and a driver of knee osteoarthritis — weak quadriceps reduce the dynamic support available to the knee during loading, increasing the stress on already-compromised cartilage. Recognizing and addressing muscle weakness around affected joints is one of the most evidence-backed components of joint health management.
9. Fatigue After Minimal Physical Activity
Joints that require significantly more muscular effort to stabilize — due to compromised cartilage, reduced proprioception, and altered joint mechanics — produce fatigue disproportionate to the activity performed. A short walk that leaves the knees feeling exhausted, or a modest workout that produces days of joint soreness, reflects a joint system that is working harder than it should to accomplish basic movement. This fatigue is often attributed to fitness level when the underlying issue is joint mechanical efficiency.
10. Posture and Gait Changes
Subtle compensations in how you walk, stand, or hold yourself — favoring one side, slightly externally rotating a foot to reduce load on a painful knee, shifting weight to avoid bearing full load through a hip — are often the earliest observable signs of joint problems. These compensations spread load to adjacent joints and muscles, creating secondary pain patterns that can eventually become as problematic as the original joint issue. If people around you have commented on changes in your walk or posture, or if you notice yourself unconsciously avoiding certain positions, your joints are communicating something worth addressing.
Risk Factors That Accelerate Joint Decline
Understanding what accelerates joint health decline helps prioritize the most impactful interventions:
- Excess body weight — Every pound of excess body weight adds approximately four pounds of force on the knee joint during walking. Weight management is the most impactful single lifestyle intervention for knee and hip joint health.
- Previous joint injury — A history of significant joint injury (ACL tear, meniscus damage, joint dislocation) increases osteoarthritis risk in that joint by 3–5 times. Post-injury joint support is particularly important.
- Sedentary lifestyle — Cartilage receives nutrients from synovial fluid through the compression and release of movement. Prolonged inactivity impairs cartilage nutrition and accelerates degradation.
- Repetitive high-impact activity — High-volume running, jumping, or repetitive occupational joint loading accelerates cartilage wear when not managed with adequate recovery and joint support.
- Chronic systemic inflammation — Inflammatory dietary patterns, metabolic syndrome, and chronic stress drive the inflammatory environment that accelerates joint tissue degradation.
- Age — Cartilage repair capacity declines with age, and the cumulative effect of decades of joint loading becomes increasingly apparent after 40.
Natural Support Strategies for Joint Health
For people in the early to moderate stages of joint health decline, several evidence-based strategies can meaningfully slow progression and improve daily comfort:
- Maintain a healthy weight — The most impactful single intervention for load-bearing joints. Even a 10% body weight reduction produces a 40–50% reduction in knee joint forces during walking.
- Strengthen the muscles around affected joints — Quadriceps strengthening for knee health, hip abductor strengthening for hip and knee alignment, and rotator cuff strengthening for shoulder health all reduce joint load during movement.
- Anti-inflammatory diet — Omega-3 fatty acids, antioxidant-rich vegetables, and limited refined carbohydrates reduce the systemic inflammatory load that drives joint tissue degradation.
- Regular low-impact movement — Swimming, cycling, and walking maintain cartilage nutrition through synovial fluid circulation without the high-impact loads that accelerate wear.
- Topical anti-inflammatory support — Directly applied compounds including Arnica, Hyaluronic Acid, and botanical anti-inflammatory extracts deliver localized support to symptomatic joints without systemic side effects.
For targeted topical joint relief, I've reviewed ArthroMax+ Cream in depth on this site. Its formula combines Arnica Oil, Hyaluronic Acid, Tea Tree Oil, Boswellia, and MSM to address joint pain, inflammation, and lubrication simultaneously through direct topical application — a practical daily support option for the specific joints causing the most discomfort.
When to See a Doctor
While many early joint symptoms respond well to natural and lifestyle interventions, the following warrant professional evaluation:
- Sudden severe joint pain without clear cause
- Joint swelling accompanied by fever — may indicate infection or systemic inflammatory disease
- Joint pain accompanied by significant morning stiffness lasting over an hour — may indicate rheumatoid or other inflammatory arthritis requiring specific treatment
- Locking or giving way of a joint during normal activity
- Rapidly progressive loss of range of motion or function
- Joint pain in a child or young adult without a clear injury history
X-ray, MRI, and blood tests (including inflammatory markers and rheumatoid factor) can identify the type and stage of joint condition, guiding appropriate intervention. Early diagnosis of inflammatory arthritis in particular enables treatment that can dramatically reduce joint damage compared to delayed diagnosis.
The Bottom Line
Joints communicate their need for support through a recognizable set of signals — stiffness, pain patterns, mechanical sounds, swelling, and functional limitations that develop gradually and compound over time. These signals are not simply inevitable consequences of aging to be accepted without response. They are meaningful biological information about the state of cartilage, synovial fluid, and surrounding tissue — information that is most useful when acted on early.
The window for meaningful intervention is widest at the earliest stages. Recognizing three or more of the signs covered in this article is a practical cue to begin the lifestyle, dietary, and targeted support strategies that can genuinely slow joint health decline and preserve function for the long term.